How are the results of clinical trials applied? In this blog post, we explore what happens to the data post-trial, and how it can be used.
A clinical trial can generate a huge amount of data. Collecting, storing and managing that data is challenging, especially for large, complex, multi-site and multinational trials. There could be millions of pieces of data by the end of a trial spanning several years, and together that data tells the story of the intervention on trial.
The scale of the data challenge has become easier to deal with now that there are Electronic Trial Master Files (eTMFs) available, such as the eTMF provided by Siron Clinical’s partner Montrium. During the trial, the data collection and storage will be monitored closely, and any questions will be resolved before the trial is closed. This ensures the data is reliable and can be used beyond the trial.
So what happens next, after the trial is closed? And who uses the results?
Publishing Clinical Trial Results

In many countries, clinical research organizations are required to publish their clinical trial results. The most common way to do this is in the form of a peer-reviewed paper in a reputable academic journal. To publish clinical trial results in a journal, you first need to analyze the results and draw conclusions from them. A paper will typically introduce the trial and its methodology and introduce and discuss some of the results.
Publishing in a journal means the research and data are peer reviewed – checked by experts in the field – and are therefore shown to be reliable. A peer-reviewed paper is generally aimed at the scientific or medical community rather than the general public.
Importantly, publication is for all clinical trial results – including negative ones. In the scientific literature, clinical trials with positive results tend to be over-represented, because of the preference for publishing positive results. This has resulted in a positive publication bias. However, negative results are just as important for the knowledge base, and journals are increasingly encouraging their publication.
Data can also be published or shared in repositories for researchers to access and analyze without the need for a full peer-reviewed article.
Global Requirements
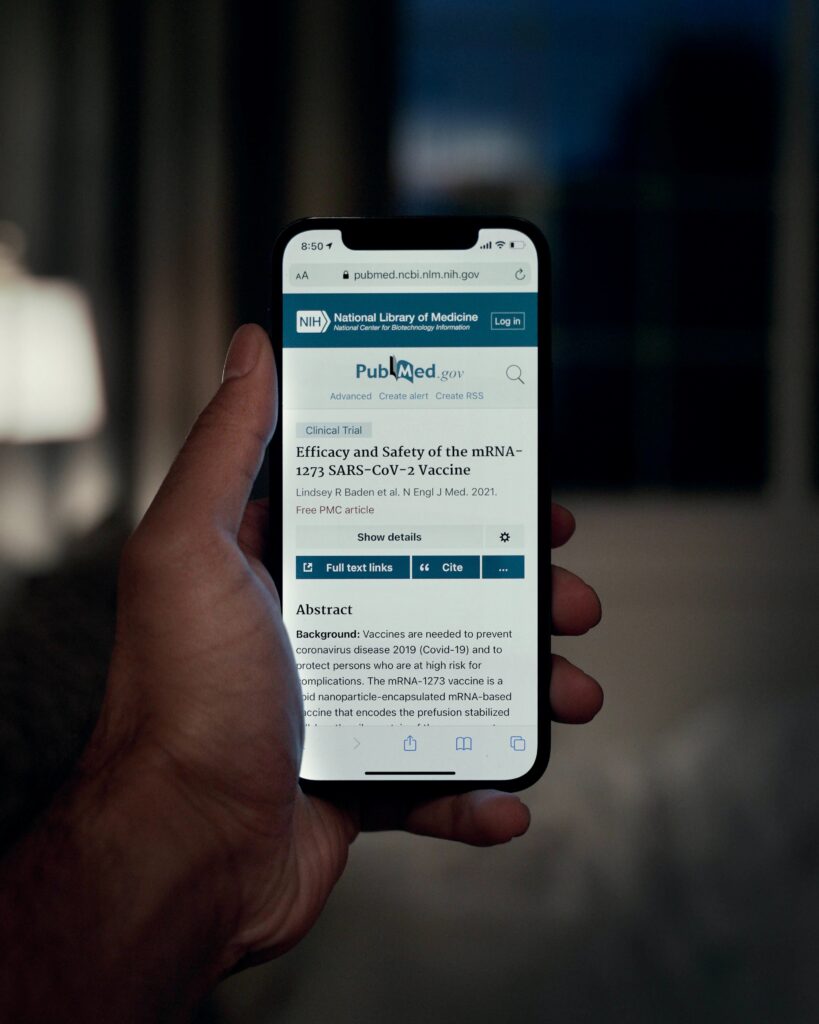
Publishing results and data isn’t just desirable; in many cases it’s a requirement. The FDA requires clinical trials to be registered and the results posted on clinicaltrials.gov. The EMA publishes clinical trial data that pharmaceutical companies submit as part of their applications. They do this for three reasons: to avoid duplication of trials and encourage innovation and the development of new medicines, to build public trust, and to give academics the chance to re-analyze data.
The WHO also has requirements for publishing clinical trial data: results must be published open access within 12 months in a peer-reviewed journal or made publicly available within 24 months, and they must be posted on a clinical trial registry within 12 months.
Beyond official requirements, campaigns like AllTrials aim to encourage transparency in clinical research. The AllTrials petition, which calls on regulators to ensure all trial results are published, has been signed by 747 organizations and almost 100,000 people.
Using The Data For Further Study
Despite regulatory mandates and public pressure, research suggests less than half of trials publish their data. This can be extremely costly for the industry. For example, if negative results are not shared, another group may unsuccessfully carry out the same trial, not realizing it had already been done.
The medical research community is currently tackling a problem known as the replication crisis. Partly due to the lack of transparency in medical research until relatively recently, it is increasingly apparent that the results of clinical trials can often not be replicated. In other words, we’re not sure if the results are correct – and sometimes therefore whether the treatments work as well as we thought.
One of the reasons for publishing clinical trial data and results is it gives other researchers the chance to re-analyze the data and even to replicate the trial. Replicated results that back up the original findings strengthen the results.
The Role Of Results In Getting Authorization

It’s not just researchers who use the data; the regulators themselves, including the EMA and the FDA, need to see the results in order to make decisions about the authorization of the treatment on trial. The results of the trial provide the evidence a treatment needs to be approved and marketed.
Ultimately, the results of clinical trials should benefit patients. It’s therefore important to make the data available for not only researchers and the authorities, but for physicians and the patients themselves. As a study in the journal Trials concluded, “Clinicians, patients, researchers and those who pay for health services are entitled to demand reliable evidence demonstrating whether interventions improve patient-relevant clinical outcomes.”
Find out more about how Siron Clinical can support your clinical trial.




0 Comments